Did you just find out that you’re going to be induced?
Do you want to know what it entails and what to expect?
You are in the right place! I have personally induced over 500 women!
In this post, you will learn:
- What an induction of labor is and what to expect,
- How your labor gets induced, and
- How long a typical induction of labor takes.
Are you excited?
Let’s get started.

What to expect when you’re being induced
When you are being induced there are several things you should expect:
- Expect the entire process to take anywhere from 24-48 hours.
- Depending on the type of induction, expect to have regular painful contractions (every 2-3 minutes).
- Expect to have a vaginal exam every 4-6 hours.
- Expect to have electronic continuous monitoring of your baby’s heart rate.
- Expect to not be able to eat solid foods (you will likely be placed on a clear liquid diet)
- Expect to not be able to walk around after your cervix reaches a certain level of dilation or after your amniotic membranes have been ruptured.
- You may or may not be able to have a support person in the room, especially because of the pandemic.
Okay, now that we have that out of the way, let’s go over all of these in a lot more detail.
How long does it take to give birth after being induced?
An induction of labor can take anywhere from 12 to 24 hours until your baby is born. If you include cervical ripening, the entire process can take 48 hours or more.
Unfortunately, it is impossible to predict how long it will take for you, but we do have standard averages.
It also largely depends on the type of induction you are having.
The different types of induction Methods
There are many different ways we can induce your labor.
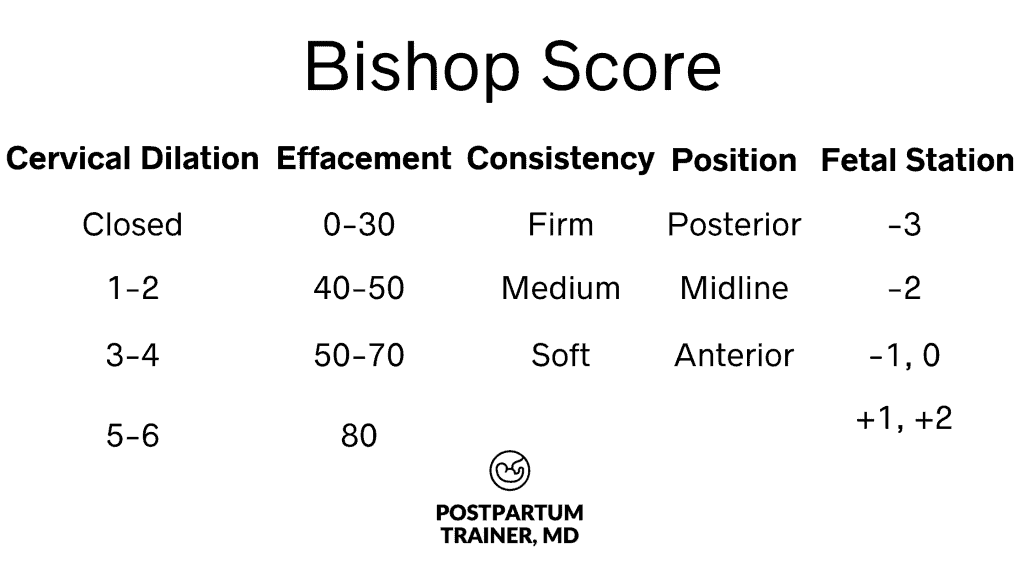
The most important factor to determine which induction agent to use is your Bishop Score.
The Bishop Score takes into account:
- How many centimeters dilated you are,
- How effaced your cervix is, (or how thin your cervix is; it’s normally thick)
- The position of your cervix (is it way back posterior, more mid-position, or anterior)
- The consistency of your cervix, (is it firm, medium, or soft), and
- The station. (how low is the fetal head relative to your pelvic bone).
Based on these 5 factors, your physician will determine a numerical value from 0 – 13.
| Score | Dilation | Effacement | Consistency | Position | Station |
|---|---|---|---|---|---|
| 0 | Closed | 0-30% | Firm | Posterior | -3 |
| 1 | 1-2 | 40-50% | Medium | Mid | -2 |
| 2 | 3-4 | 60-70% | Soft | Anterior | -1,0 |
| 3 | 5-6 | 80% | – | – | +1 |
A value greater than 6 indicates a “favorable cervix” meaning you are more likely to have a successful induction.
A value less than 6 indicates a “less favorable bishop score” signifying that your chance of successful vaginal birth is decreased.
If your bishop score is less than 6, we will need to first ripen your cervix. In other words, we try to soften and prepare your cervix for dilation.
Let’s talk about how we do that.
Prostaglandin Medications
Prostaglandins are the most commonly used medications for ripening or preparing your cervix for labor induction.
There are two types of prostaglandin medications:
- Misoprostol, also known as Cytotec, and
- Dinoprostone, also known as Cervidil
Cytotec
Cytotec is a prostaglandin E1 analogue that helps to soften the cervix and it often causes uterine contractions.
This medication comes in pill form and could be placed in the vagina or under the tongue.
It could be given every 3-4 hours for a maximum of 6 doses.
I do want to say, this medication is contraindicated if you are attempting a trial of labor after cesarean (TOLAC).
Cervidil
Cervidil is a prostaglandin E2 analogue that is meant to soften the cervix. It may cause dilation and contractions as well.
This medication looks like a small skinny tampon with a long string, and it is placed deep into the vagina to start the ripening process.
The cervidil will be removed:
- if you begin dilating,
- if you begin contracting excessively,
- or if 12 hours have passed (whichever comes first).
Aside from medications, we also have another way to dilate or ripen the cervix.
Mechanical Dilation
Mechanical dilation uses pressure to dilate your cervix, rather than medications.
This can be done using a:
- Cook balloon, or
- Foley catheter balloon
One of these balloons will be inserted into your cervix and the balloon will be filled with sterile water.
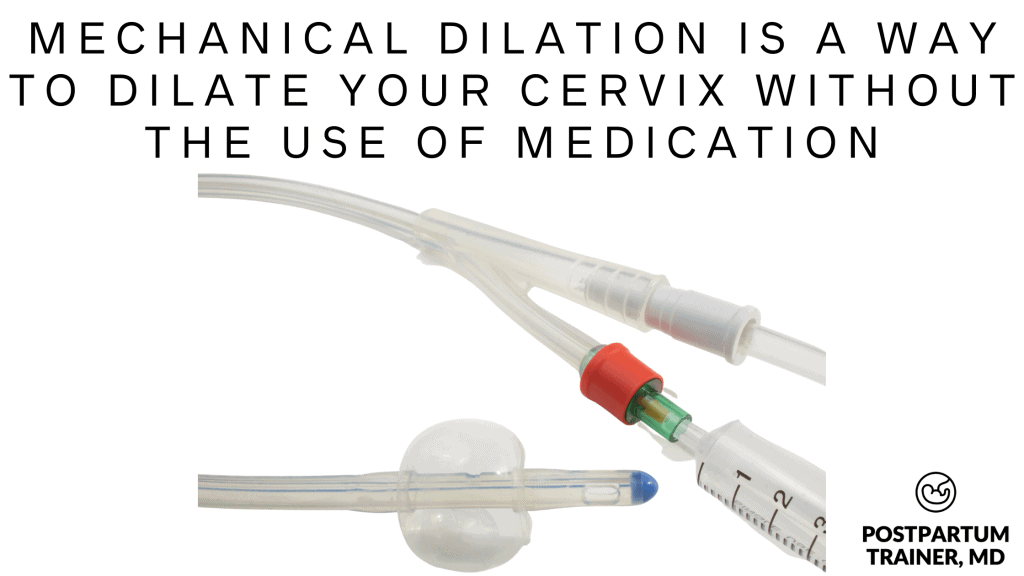
You may feel a lot of pressure as the balloon is filling. So if you eventually want an epidural, feel free to get one prior to balloon placement.
The balloon will stay inserted in the cervix until your cervix is about 4 centimeters dilated or after 12 hours (whichever comes first).
A mechanical dilation is a great option for:
- women who are about 0.5-1 centimeter dilated, and/or
- for women who cannot receive additional prostaglandin medication.
It is also a great option if you are considering a trial of labor after cesarean (TOLAC).
Okay, so that’s how to ripen the cervix and get a couple of centimeters of dilation.
Now let’s get to the full-blown induction.
Uterotonic Medications
The most commonly used uterotonic mediation is oxytocin also known as Pitocin.
Oxytocin is a hormone that is normally released by the posterior pituitary gland when the onset of labor occurs and also during breastfeeding.
We give it through the IV to either initiate uterine contractions or augment your labor.
Pitocin mostly works at the uterine receptors to increase the frequency, duration, and amplitude of your contractions.
Once you are on oxytocin, most hospitals will not allow you to eat in case of an emergency (i.e needing an urgent cesarean section).
And last but not least we have another intervention up our sleeve…
Amniotomy
Amniotomy is a process in which we “break your water.” This is known as AROM, or artificial rupture of membranes.
This is a bedside procedure that occurs using a small hook to pierce the amniotic sac which causes the amniotic fluid to leak out.
Don’t worry this will not hurt!
After an amniotomy, you will continue to leak- this is completely normal.
Sometimes, an amniotomy alone can get your contractions going. But we often use this in conjunction with pitocin to achieve a regular contraction pattern.
So those are all the ways in which we can induce your labor starting from a closed cervix.
Now let’s talk about timing.
How Long Does An Induction Take (Step By Step)
As I mentioned before, an induction of labor can take upwards of 48 hours in first-time moms and up to 24 hours in women who have given birth before.
Let’s discuss the three stages of labor and how long each one takes.
Inducing The First Stage of Labor
The first stage of labor corresponds to when you are 0 cm dilated, to 10 cm dilated.
It is broken up into 2 parts, the Latent Phase & The Active Phase
The Latent Phase
The latent phase is the time it takes to get from 0 – 6 centimeters.
- This can take up to 20 hours in primiparous women aka, first-time moms and
- Up to 14 hours in multiparous women aka women who have had a prior delivery.
Yes, I know what you are thinking, it is a long time.
But you have to understand that your cervix and body weren’t yet ready for labor.
You really must be patient during this stage of labor and stay positive.
The Active Phase
Active labor occurs from the time you reach 6 centimeters to the time you are fully dilated or 10 centimeters.
- This stage can last anywhere from 0 – 6 hours on average depending on your parity.
For multiparous women, this stage can be very short!
There have been so many instances where I have seen women go from 6 centimeters to fully dilated in less than an hour.
The Second Stage of Labor
The second stage of labor occurs from full dilatation to delivery of the fetus.
This stage could last anywhere from 1- 4 hours depending on if you are nulliparous or multiparous, the type of pelvis you have, the position of the baby, and whether or not you have an epidural.
Some providers will have you start pushing as soon as you reach full dilatation whereas others will allow you to “labor down.”
Laboring down is a process in which you allow the fetal head to descend further down into the pelvis before you start pushing.

The thought process is that laboring down will help prevent you from pushing for hours, which can tire you out.
Believe it or not, the average time it takes to push a baby out is 90 minutes! It’s not instantaneous like you see in the movies.
To learn more about pushing, how to push effectively, and exercises you could do to prepare you for labor, click here.
The Third Stage of Labor
The third stage of labor occurs from delivery of the fetus to delivery of the placenta.
This should take no longer than 30 minutes.
If after 30 minutes the placenta does not deliver the placenta has to be removed manually.
Your provider will either manually deliver the placenta at the bedside, or take you to the operating room to surgically remove the placenta to reduce your risk of postpartum hemorrhage and infection.

Here is a table of how long a normal induction of labor can take.
| Stage of Labor | Nulliparous Woman | Multiparous Woman |
|---|---|---|
| Cervical Ripening | Up to 12 hours | Usually not needed |
| Latent Phase of Labor (0-5 cm dilated) | Up to 20 hours | Up to 14 hours |
| Active Phase of Labor (6-10 cm dilated) | ~ 6 hours | 0-6 hours |
| The Second Stage (Delivery of the baby) | 1-4 hours | 0-3 hours |
| The Third Stage (Delivery of placenta) | Up to 30 min | Up to 30 min |
The Immediate Postpartum
The fourth stage of labor has been described by some to be the immediate postpartum period.
During this time your provider will:
- assess the tone of your uterus to ensure it has started to contract down.
- assess and repair any lacerations.
- assess your vital signs including blood pressure and heart rate.
- assess the amount of uterine/vaginal bleeding you are experiencing.
This is one of the most important phases of labor as hemorrhage is one of the leading causes of maternal morbidity and mortality in developed and developing nations.
Is induced Labor more painful Than Natural Labor?
Induced labor can be more painful than natural labor.
Pitocin often causes stronger, longer, and more frequent uterine contractions than natural contractions.
Oftentimes, women will get an epidural due to the intensity of the pain.
With that said, I have seen plenty of women get induced without pain medication.
It is possible!
However, I always tell my patients, if you are in pain and you cannot tolerate the pain it is OKAY to have pain relief.
YOU DON’T HAVE TO BE A HERO OR PROVE ANYTHING TO ANYONE.
Getting a break from the pain of the contractions could help you relax and get some rest before needing to push.
Can I Get An Epidural Before The Induction?
You can get an epidural at any point in your induction!
There is no minimum number of centimeters dilated you need to be.
I do want to say however, you must be able to sit still for epidural placement.
So please don’t wait until the pain is so severe that you are unable to sit still.
Also, once you get the epidural, you will be confined to the bed. So no more walking around.
Is being induced harmful to the baby?
The actual induction of labor is not harmful to the baby, however, your baby may not tolerate the frequent contractions.
This is why you will be connected to an electronic fetal heart rate monitor when we start your induction.

The baby communicates with us through its heart rate.
If the baby is in distress, we will know.
Unfortunately, all medications used for induction of labor have side effects and because of that, we need to keep a close eye on your baby’s heart rate tracing.
Do you stay in the hospital after being induced?
Yes, you will be admitted to the hospital for an induction of labor and will stay in the hospital for at least 1-2 days postpartum or 2-4 days post-c-section.
We must monitor you in the early postpartum period to check your bleeding, your blood pressure, and incision if you had a cesarean delivery.
Other Related Questions
Is induction easier if you are already dilated?
Yes, an induction of labor is easier if you are already dilated. The more dilated you are, the more favorable your Bishop Score will be.
If your Bishop Score is 6 or greater, your induction is more likely to be successful than if you have a closed cervix giving you a bishop score of less than 6.
When you are dilated, we do not need to spend time ripening and preparing the cervix for labor as it is already dilated.
In this case, we can jump straight to the induction agents.
**Also if you have had a vaginal delivery in the past, your induction is more likely to be easier and faster.**
How long does induction take for the second baby?
An induction of labor is usually much quicker for a second baby compared to the first. On average, it can take up to 12-24 hours for second-time moms to give birth after induction.
Why do doctors push inductions?
The most common reason why doctors push inductions is for a medical indication.
Our goal is “healthy mom & healthy baby.”
Inductions are recommended when we determine that it is no longer beneficial for you or your baby to remain inside the uterus.
We want to do everything in our power to ensure the health and wellbeing of both you and your baby.
Are there natural ways to induce labor?
The most effective, natural way to induce your labor is known as membrane sweeping.
Membrane sweeping can be done during a vaginal exam if your cervix is at least 1 cm dilated.
It refers to physically separating the amniotic sac / membrane from the cervix with a finger sweep.
This should only be performed by a doctor or a midwife, and ONLY after you reached full term (39 weeks). That’s because a membrane sweep can lead to uterine contractions and possible rupture of the amniotic membranes.
Aside from membrane sweeping, some providers will encourage women to walk to help induce labor.
Although there haven’t been many scientific studies to prove this, walking is a great way to exercise during the third trimester. I talk about this more in walking to induce labor.
Is inducing labor at 39 weeks safe?
39 weeks is considered full-term. Induction of labor is very safe for you and your baby at this time.
37 – 38 weeks gestation is considered early term and thus we do not electively induce labor at this time.
In fact, there was a famous study done in 2018 called the ARRIVE Trial which compared outcomes in low-risk women at 39 weeks to an elective induction of labor or allowing them to go into spontaneous labor.
This trial showed a decreased rate of cesarean delivery in those women who were electively induced at 39 weeks compared to the women who were expectantly managed.
Is it safe at 38 weeks or less?
The only reason we would induce you prior to 39 weeks is if you have a pregnancy or fetal condition that can have negative consequences by prolonging your pregnancy.
Common examples include:
- Gestational Diabetes
- Gestational Hypertension
- Premature Rupture of Membranes
- Preeclampsia
- Chronic Hypertension
- Cholestasis of Pregnancy
- Growth Restricted Baby
- Twins
- Low Fluid
Do’s and Dont’s Before Being Induced
I do want to mention there are many things that people will tell you to do to induce your labor but have not been proven to be effective.
The following is a list of methods that are not proven or recommended:
- Nipple stimulation
- Castor oil
- Primrose oil
- Spicy food
- Massage
- Acupuncture
Now let’s talk about what you should do.
What Should I Do The Day Before Labor Induction?
The day before your induction of labor should be spent doing something for yourself.
Especially if this is your first baby!
Go out to eat with your partner as you may not be able to eat in labor, take a nice stroll as you may be stuck in bed for hours on end, or watch a movie.
Just do something that is relaxing and not stressful.
You should also make sure your baby bag is packed and you have everything you need for the hospital.
Don’t forget to pack a comfortable pair of slippers, possibly your favorite pillow and/or blanket, and chapstick as your lips get extremely chapped when pushing!
What Are The Disadvantages and Risks of Induced Labor?
I do want to mention that inductions of labor can be associated with some risks and disadvantages.
Those risks include:
- Infection
- Tachysystole (Frequent contractions)
- Failed induction
1. Infection
When you are admitted to the labor floor, typically you will have a cervical exam every 4-6 hours depending on the institution, to assess for change.
If you are being induced for 24-48 hours that can be a lot of examinations!
Although we are using sterile gloves, the vagina has A LOT of bacteria including group b streptococcus (GBS) that is present in some women. Thus, each time we examine you there is a risk of introducing bacteria into the uterus.
The risk of infection is further increased if your amniotic membranes have been ruptured for several hours.
To decrease the risk of infection, most physicians will limit the number of examinations you receive while in labor and/or give you antibiotics if you are found to be GBS positive.
2. Tachysystole
Tachysystole is defined as having too many uterine contractions, too close together.
The actual definition is the presence of more than 5 uterine contractions in a ten-minute period averaged over 30 minutes.
Tachysystole is considered a risk of induction because it can cause your baby to become distressed.
Think about it- as the uterus contracts the baby, placenta, and umbilical cord are getting squeezed.
During tachysystole, the baby only has about one minute of relaxation to “catch its breath.”
Some babies do fine and can tolerate it, whereas other babies cannot.
If your baby is in distress, we can give medication to relax the uterus to allow your baby more time to recover.
3. Possible need for cesarean section
Once we start an induction – the clock has started.
Depending on how many centimeters dilated you are, you have to show signs of progress. If you are not, you will need a c-section.
With that said, the need for a cesarean section can occur even if you don’t have an induction.
Studies show that there is no increased risk of cesarean section during an induction of labor.
Final Words on Labor Induction
So there you have everything you need to know about labor induction.
Do you feel ready?
Now I want to hear from you.
Did you have your labor induced, or are you scheduled for an induction?
What was your experience like or what are you most worried about?
Comment below and let me know!
Related Posts on Pregnancy
- 10 Unique Exercises to Prepare You For Labor
- Does Walking Help to Induce Labor
- What Muscles Are Cut During C Section
References:
- Zhang J, Landy HJ, Ware Branch D, et al. Contemporary patterns of spontaneous labor with normal neonatal outcomes. Obstet Gynecol. 2010;116(6):1281-1287. doi:10.1097/AOG.0b013e3181fdef6e
- Finucane EM, Murphy DJ, Biesty LM, et al. Membrane sweeping for induction of labour. Cochrane Database Syst Rev. 2020;2(2):CD000451. Published 2020 Feb 27. doi:10.1002/14651858.CD000451.pub3
- Grobman WA, Rice MM, Reddy UM, et al. Labor Induction versus Expectant Management in Low-Risk Nulliparous Women. N Engl J Med. 2018;379(6):513-523. doi:10.1056/NEJMoa1800566
- Wood S, Cooper S, Ross S. Does induction of labour increase the risk of caesarean section? A systematic review and meta-analysis of trials in women with intact membranes. BJOG. 2014;121(6):674-685. doi:10.1111/1471-0528.12328
Get Four Free Workouts To Help Strengthen Your Pelvic Floor & Heal Your Mommy Tummy!

Brittany Robles, MD, MPH, CPT
Brittany Robles is a full-time OBGYN physician, a NASM certified trainer, and a prenatal and postnatal fitness specialist. She holds a Master of Public Health degree in maternal health with a special interest in exercise and nutrition. She is also the co-author of The White Coat Trainer. Learn more about her here.
Sharing is Caring – Send This To A Mom In Need!

I am being induced with my first child tomorrow. This article has for sure put my mind at ease, as well as giving me an idea of things to bring to keep my mind occupied while I am in the waiting phase of my induction. I am very excited for my baby to get here.
Hi Catherine,
Thank you so much for your comment.
I hope your induction went well and congratulations on the birth of your baby!